CPTSD Brain Changes: Understanding Trauma's Impact
March 10, 2026 | By Beatrice Shaw
Have you ever wondered why your reactions to stress feel so intense or uncontrollable? You might find yourself snapping at a loved one or suddenly feeling completely numb without knowing why. Why does trauma feel like it is happening right now, even if the event ended years ago?
The answer is not a lack of willpower. It lies deep within the physical structure of your brain. When you experience prolonged or repeated trauma, your brain actually changes its shape and how it functions to help you survive. These neurological shifts are the foundation of Complex PTSD (CPTSD). Understanding these changes is the first step toward validating your experience and finding a path to healing. If you are struggling with these symptoms, you can start your test to gain a clearer understanding of your current state.
This guide explores how chronic trauma impacts the brain and nervous system. By looking at the science, we can move away from "What is wrong with me?" and toward "What happened to my brain, and how can I heal?" To help pinpoint how these changes manifest in your daily life, you can take our free assessment to identify which symptoms affect you most.
How Chronic Trauma Reshapes Your Brain
When we talk about CPTSD, we are talking about a brain that has been "rewired" for survival. Unlike a single traumatic event, complex trauma involves repeated stress, often in childhood or long-term relationships. In these environments, the brain stays in a state of high alert. Over time, this constant pressure causes physical changes in specific regions that govern emotions, memory, and logic.
The Amygdala: Your Body's Overactive Alarm System
The amygdala is a small, almond-shaped part of the brain responsible for detecting threats. Think of it as your internal smoke detector. In a brain unaffected by trauma, the amygdala sounds the alarm when there is real danger, such as a car swerving into your lane. Once the danger passes, the alarm turns off.
In people with CPTSD, the amygdala becomes hyper-reactive. Because the trauma was constant, the smoke detector learned to stay "on" at all times. This leads to a state of hyper-vigilance, where you are always scanning your environment for threats. Even small things, like a specific tone of voice or a crowded room, can trigger a full-blown survival response. You aren't "overreacting"; your amygdala is simply doing the job it was trained to do during the trauma.
Hippocampus Changes and Memory Fragmentation in CPTSD
The hippocampus functions like your brain's librarian. It processes memories and adds a "time stamp" to indicate they belong in the past. This helps your brain distinguish between past memories and your current reality.
Studies show that chronic stress can actually shrink the hippocampus. When this happens, the "librarian" cannot do its job correctly. Instead of filing memories away as "past events," the brain leaves them active and disorganized. This is why survivors often experience emotional flashbacks. A smell or a sound can cause you to feel the exact terror you felt years ago because your brain cannot tell the difference between "then" and "now." Taking a cptsd test can help you identify if these memory-related symptoms are part of your experience.
Nervous System Dysregulation: The Hidden Driver of CPTSD Symptoms
The brain does not work alone; it communicates through the nervous system. When we experience CPTSD, our Autonomic Nervous System (ANS) loses its ability to return to a calm state. This is known as nervous system dysregulation. It explains why you might feel "wired but tired" or feel like you are watching your life from outside your body.
Polyvagal Theory and the Three States of Trauma Response
Polyvagal Theory, developed by Dr. Stephen Porges, helps us understand how our nervous system responds to perceived safety or danger. According to this theory, our system operates in three primary states:
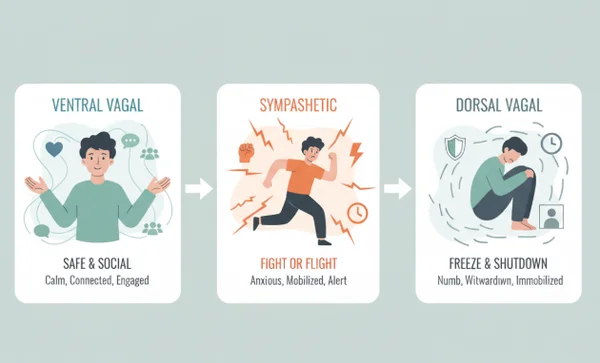
- Ventral Vagal (Safe and Social): You feel calm, connected, and curious. This is the state where healing happens.
- Sympathetic (Fight or Flight): Your heart rate increases, and you feel anxious or angry. Your body is preparing to deal with a threat.
- Dorsal Vagal (Freeze or Shutdown): If the threat is too big to fight or escape, your system "unplugs." You might feel numb, depressed, or physically heavy.
In CPTSD, the nervous system gets stuck in the Sympathetic or Dorsal states. You may find it very difficult to reach the "Safe and Social" state, even when you are with people who love you. Understanding these states can help you realize that your "laziness" might actually be a Dorsal Vagal freeze response.
Understanding the Fight, Flight, Freeze, and Fawn Responses
While most people know about "Fight or Flight," complex trauma survivors often develop two additional survival strategies: Freeze and Fawn. These are known as the 4 F’s of CPTSD.
- Fight: Responding to triggers with anger or controlling behavior to feel safe.
- Flight: Using busyness, workaholism, or literal running away to avoid emotional pain.
- Freeze: Disconnecting from the world, scrolling social media for hours, or feeling "spaced out" to numb the pain.
- Fawn: Attempting to appease or "people-please" a potential threat to avoid conflict.
These responses were once life-saving tools. However, when they persist into adulthood, they can cause significant distress in your daily life. To see which patterns you might be using, you can take the test for more personalized insights.
The Neurobiology of Self and Relationships in CPTSD
The physical changes in the brain do more than just make us feel anxious. They also change how we view ourselves and how we connect with other people. CPTSD is often called a "disorder of self-organization" because it disrupts the core of who we are.
Prefrontal Cortex Impairment and Self-Regulation Challenges
The prefrontal cortex (PFC) is the "CEO" of the brain. It is responsible for logical thinking, planning, and regulating our emotions. When the amygdala (the alarm) is screaming, the PFC often goes "offline." This is why it is so hard to "think your way out" of a panic attack.
Chronic trauma often weakens the PFC. This can make impulse control and decision-making challenging for people with CPTSD. You might feel like your emotions are driving the car, while your logical self is locked in the trunk. Strengthening the connection between the PFC and the amygdala is a major goal of trauma therapy. Evidence-based approaches like EMDR can help rewire trauma responses and restore this vital balance.
How Trauma Alters Neural Pathways for Trust and Connection
Human beings are wired for connection. However, when trauma occurs within a relationship—especially with a caregiver—the neural pathways for trust are damaged. The brain learns that "people are dangerous" or "closeness leads to pain."
This can lead to a disorganized attachment style. You might desperately want love but feel a sudden urge to push people away the moment they get close. This is a biological defense mechanism. Your brain is trying to protect you from the pain it remembers so well. Healing involves slowly teaching your brain that safe connection is possible. Using an online tool to assess your symptoms is a brave first step toward rebuilding that trust in yourself.
Rediscovering Resilience and Rewiring for Recovery
Your brain's remarkable plasticity offers real hope for healing. The same neural pathways that developed to help you survive can be rewired with safety, support, and therapeutic approaches. Recovery isn't about becoming someone you weren't—it's about rediscovering the resilience that was always within you.

You're not broken—you're a survivor with a brain that adapted to protect you when you needed it most. That same capacity for adaptation now becomes your greatest asset on the path to healing. By understanding the amygdala, the hippocampus, and the nervous system, you can start to separate your identity from your symptoms. You are not your flashbacks, and you are not your freeze response. You are a person who has survived, and your brain is capable of finding its way back to balance.
The first step in any healing journey is clarity. Once you name what you are experiencing, it loses some of its power over you. To get a detailed look at how these patterns might be showing up in your life, we invite you to see your results through our free, confidential screening tool based on the latest scientific standards.
The Takeaway
Can CPTSD brain changes be reversed?
Yes, the brain is remarkably resilient. Through a process called neuroplasticity, you can form new neural pathways. Treatments like trauma-focused therapy, mindfulness, somatic experiencing, and even consistent healthy relationships can help "calm" the amygdala and strengthen the prefrontal cortex. Healing takes time, but the physical structure of your brain can indeed shift toward a more regulated state.
How do I know if my symptoms are related to brain changes from trauma?
If you find that your emotional responses are disproportionate to the current situation—such as feeling extreme terror when someone forgets to text you back—it is likely a neurological trauma response. Other signs include persistent brain fog, inability to remember parts of your childhood, or feeling constantly "on edge" even in safe environments. Identifying these patterns through a screening test can provide the validation you need to seek professional help.
Are there tests to measure CPTSD-related brain changes?
While researchers use MRI and PET scans to see these changes in clinical studies, these are not typically used for individual diagnosis. Instead, professionals use clinical interviews and validated questionnaires based on the ICD-11 standards. Our online screening is designed to help you see if your experiences align with the recognized symptoms of CPTSD, providing a starting point for your recovery journey.
Disclaimer: This article is for educational purposes only and does not constitute a medical diagnosis. If you are in crisis or struggling with severe symptoms, please reach out to a qualified mental health professional or a local crisis hotline.